Dry needling is a modern therapy for treating different kinds of pain. It has been proven that dry needling therapy is most beneficial for muscle-related pain.
Dry needling and acupuncture are both effective therapies for short-term pain relief. Both methods use the same equipment.
However, what about performing dry needling for tendonitis? Numerous studies have confirmed the immediate effectiveness of dry needling for chronic tendon injury.
Dry needling therapy stimulates blood flow to the injured area, triggering stem cell recruitment, stimulating fibroblasts, and inducing the healing cascade. For tendon tears, giving autologous blood injections increases the chances of tendon healing.
The best way to reduce pain and treat tendon injuries is to perform dry needling in conjunction with physical therapy. That way, the treatment will yield a maximum increase in strength and the joint’s range of motion.
Can Dry Needling Help Tendonitis
Tendons generally have a poor blood supply, which is why they are vulnerable to vascular compromise in specific areas. There is substantial evidence that dry needling treatment for tendinopathy is beneficial. Some studies suggest that this previously mentioned therapy can help with injuries related to wrist common extensor origin, patellar tendon, rotator cuff, and tendons around the greater trochanter. In the following sections, we will provide studies and evidence that either supports its efficacy or show no significant improvements.
Dry Needling Treatment for Achilles Tendonitis
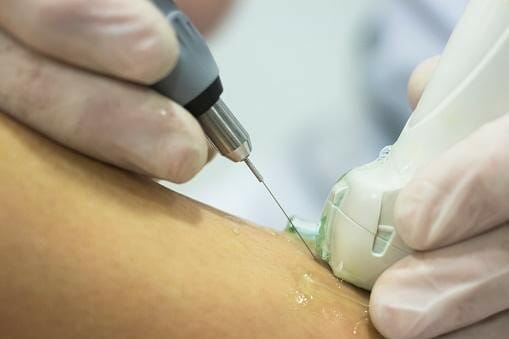
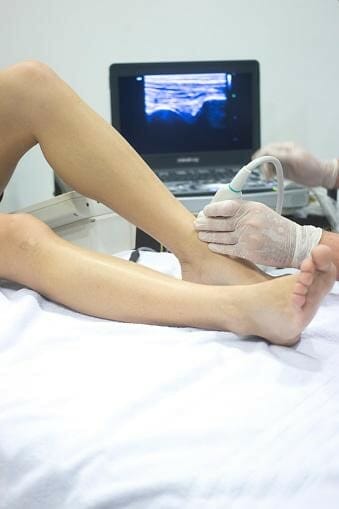
First, the dry needling practitioner scans the injured area with ultrasound to evaluate the condition of the tendon. The next step is to clean the skin with an antiseptic thoroughly. Sometimes the practitioner will inject a local anesthetic into the skin of the injured area of the Achilles tendon. The main focus of the previous step is to make the procedure more comfortable.
Finally, dry needling is performed under ultrasound guidance. Ultrasound ensures precise needle penetration. The practitioner will repeatedly pass the needle through the injured tendon’s area to cause small bleeds. In turn, small bleeds will stimulate the healing factor and flow of nutrients. In addition, some cases require autologous blood to increase the chances of a faster healing process.
A prospective, double-blind study with 50 participants evaluated the effectiveness of peritendinous autologous blood injections. The study’s subjects were patients with mid-portion Achilles tendinopathy. The main measurement was the Victorian Institute of Sports Assessment-Achilles (VISA-A) score. The results show that both groups significantly improved the VISA-A scores, but there was no significant difference between the groups.
Dry Needling for Tennis Elbow
In the double-blind study, 230 participants evaluated the clinical value of dry needling for the treatment of tennis elbow. The study has shown statistically significant changes in both the active and the placebo groups. There were no major changes between groups in 12 weeks, but significant improvements were noticed in the active group after the 24 weeks.
Another study tried to evaluate if treatment methods with autologous conditioned plasma (ACP) has advantages over classical ultrasound-guided dry needling. There was a 34% reduction of VAS in the dry needling group and a 48.5% reduction in the ACP group. The authors concluded that more significant clinical improvements are seen in the patients treated with additional ACP.
The third study compared the outcomes of dry needling and first-line treatment consisting of ibuprofen 100 mg twice a day and a proximal forearm brace. Ninety-two patients completed the study, and all were diagnosed with lateral “epicondylitis.” The first-line treatment group has shown no significant improvements. In contrast, the dry needling group proved effective at three weeks and six months. The authors suggest that dry needling is a safe and effective treatment method for lateral “epicondylitis.”
Dry Needling for Rotator Cuff Tendinopathy
In one of the double-blind RCT studies, the effects of tendon needling were studied, and 30 patients participated in total. The authors tried to evaluate the effects of tendon needling with an injection of PRP and without it. The primary measurement was the Shoulder Pain and Disability Index. Both treatments were performed twice with a 4-week interval between injections.
Significant improvements were demonstrated in both groups, but PRP injections proved to be more beneficial when it comes t
o symptomatic relief and functional improvements. However, there were no significant improvements in the shoulder range of motion.
Dry Needling for Patellar Tendonitis
One double-blind study evaluated tendon needling with or without the addition of PRP in patellar tendinopathy. A total of 23 patients were included, and all failed nonoperative treatment. The groups underwent ultrasound-guided tendon penetration ten times in total, with or without the addition of PRP. The primary measurement was the VISA score.
Both groups have shown improvements in the VISA scores. However, the PRP group had improved significantly more than the dry needling group. The biggest differences were captured at 12 weeks, but no differences between groups were noticed at 26 weeks. In conclusion, the addition of PRP in patellar tendinopathy showed significant improvements in the 12-week period compared to the dry needling group, but the differences disappeared after 26 weeks.
Dry Needling for Greater Trochanteric Pain Syndrome
The single-blinded study aimed to compare ultrasound-guided percutaneous tendon dry needling to PRP injection to treat greater trochanteric pain syndrome. A total of 30 patients with gluteus medius/medius tendinosis participated. During the study, patients were carefully monitored, but care after treatment was not controlled. The main measurement was pain scores assessed at approximately 1 and 2 weeks. The results show that both groups showed major improvements in pain scores.
What are autologous blood injections?
Autologous blood injection draws a small volume of venous blood from the patient and then re-injects it in and around the tendon origin. ABI is a treatment option for chronic tendon inflammation like tennis/golfers elbow, Achilles tendinitis, and patella tendonitis. As opposed to Platelet Rich Plasma(PRP), there is no blood preparation. Also, unlike PRP, ABI is not for early-stage osteoarthritis, bursitis, or other forms of joint inflammation.
Dry Needling and Physical Therapy for Treating Tendonitis
Combining physical therapy with dry needling in Philadelphia, PA is the best way to treat tendonitis, reduce and relieve pain, and recover from a tendon injury. First, physical therapy aims to improve the strength of the muscles affected by the related tendonitis. That is followed by the restoration of the primary function in the joint. Pain reduction will follow after a couple of dry needling sessions and physical therapy.
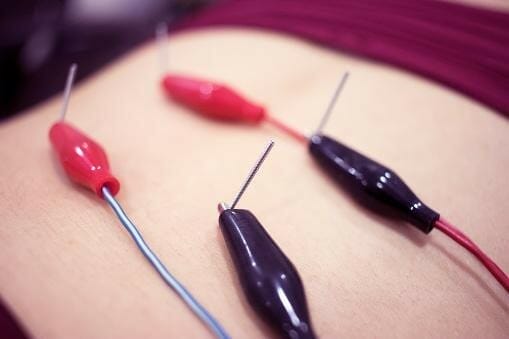
Muscles contract and relax when a practitioner targets trigger points. Inserting and removing the needle produces a stimulative effect inside the muscle. In addition, the result is immediate muscle relief of tightness and pressure. Lastly, pain and inflammation are either eliminated or greatly reduced.
Dry Needling Side Effects
Most of the time, dry needling has no severe side effects. However, there are some mild ones people may experience.
Here are some of the dry needling side effects:
- Temporary increase in pain – Usually occurs 24 to 48 hours after the session.
- Bruising or bleeding – These two occur at the insertion site.
- Fainting – Most likely to affect athletic men, older or weaker individuals, middle-aged women, and dehydrated people.
- Fatigue and tiredness – Rare, but some people may experience them.
- Skin reactions – Reactions are in the form of small red spots.
- Pneumothorax – Collapsed lung is extremely rare and can be avoided by only seeking certified and experienced practitioners.
Conclusion
There is substantial evidence that dry needling treatment is beneficial for tendonitis.
Evidence suggests that dry needling is effective for treating:
- tennis elbow
- rotator cuff tendinopathy
- Achilles tendinopathy
- patellar tendinopathy
- greater trochanteric pain syndrome
It has been proven that combining dry needling treatment with physical therapy is the best way to treat chronic tendinosis and relieve pain. Strengthening the muscles will increase the chance of faster healing and fully restoring the joint’s primary function. Combining these two treatments will reduce the pain and inflammation after only a couple of sessions.
If you are in the Bryn Mawr or Haverford, PA area and are interested in exploring Dry Needling therapy as a treatment method, please call or schedule a consult!